January 15, 2019

When the Price Is Right: Aligning Payment with Health System Transformation
In 1952 at the tender age of 25, Elizabeth became the Queen of England upon the death of her father King George V. The popular Netflix series “The Crown” depicts the early years of Queen Elizabeth II’s reign as she assumed her new responsibilities, and the monarchy adapted to a modernizing post-war world where many questioned its continued relevance.
Queen Elizabeth’s skill in transforming the Crown’s relationship with the British people has kept the monarchy intact and relevant. The Queen’s adaptability to changing circumstances has been essential to her long-term success.
Like the British monarchy in the 1950s, U.S. healthcare today confronts a daunting transformational challenge as Americans are demanding greater price transparency, care coordination, convenience and value. The old ways of delivering and paying for healthcare are unsustainable and not supported by the American people. It’s “adapt or die” time for America’s healthcare industry. Health companies that find new and better ways of connecting with customers in the post-reform marketplace will lead a revolutionary industry transformation. That revolution begins and ends with meeting customer needs, wants and desires.
ROYAL “ADAPT OR DIE” TIME
The 1950s was a period of profound social change for Great Britain. Devastated by German bombing and catastrophic human losses during World War II, the country needed to rebuild. At the same time, the English people began a euphoric rush into a modernizing world characterized by economic prosperity, greater personal freedom, changing cultural values and television. 
As Elizabeth assumed the throne, the British monarchy was out of step with the British people. Resolutely tradition-bound and rigid, it carried on as though nothing had changed. Its inability to connect meaningfully with its subjects threatened its relevance and sustainability. This became apparent in 1956 when a routine speech at a Jaguar factory triggered a constitutional crisis regarding the monarchy’s role in British Society.
Clearly bored, Queen Elizabeth read the following lines to the Jaguar workers,
“We understand that in the turbulence of this anxious and active world, many of you are leading uneventful, lonely lives where dreariness is the enemy. Perhaps you don’t understand that on your steadfastness and ability to withstand the fatigue of dull, repetitive work depend, in great measure, the happiness and prosperity of the community as a whole.
The upward course of a nation’s history is due, in the long run, to the soundness of heart of its average men and women. May you be proud to remember how much depends upon you and that even when your life seems most monotonous, what you do is always of real value and importance to your fellow countrymen.”
To people weary of sacrifice, this stiff upper lip rhetoric no longer resonated. Lord Altrincham, the same age as the Queen and a staunch monarchist, heard the speech in a packed dentist’s waiting room. The lack of interest in and respect for the Queen’s remarks appalled him, but he believed the Queen herself was primarily responsible the monarchy’s declining public support.
Altrincham wrote a widely-circulated and controversial critique of the Queen’s public persona and speaking style. He encouraged her to recognize that Britain had changed, and that she and the monarchy needed to become more accessible and contemporary. He ended a nationally televised interview with this prescient warning,
“Until recently, monarchies were the rule and republics the exception, but today, republics are the rule and monarchies very much the exception.”
To her credit, Queen Elizabeth internalized the criticisms and initiated sweeping changes to improve her connection with the British people. She abolished the practice of introducing debutantes, televised her annual Christmas Message and opened Buckingham Palace to the British people.
Unlike most monarchies that have atrophied or vanished during the last century, the British Crown continues to prosper as it adapts to an ever-changing world. In Prince Harry’s larger-than life royal wedding on May 19, 2018, the Queen warmly welcomed once-divorced American Meghan Markle into the royal family. This was a sharp contrast to the traditional royal practice of forbidding marriage with divorcees. The Queen’s uncle Edward VIII abdicated the throne to marry once-divorced Wallis Simpson, and the Queen herself forbade her sister Margaret to marry her divorced fiancé Peter Townsend. How times change.
The royal family adapts and so too must U.S. healthcare. In the same way Elizabeth deepened her connection with the British people, so too must health companies deepen their customer connections. The road to post-reform success requires price transparency, empathy and respect. There are no shortcuts.
THE PRICE IS WRONG
Healthcare costs in America have risen steadily and alarmingly. Many Americans can no longer afford healthcare, even with insurance, because wages have not kept pace with inflation, and copays and deductibles have become unmanageable.
Healthcare’s artificial economic model separates patients (i.e. consumers) from the purchasing and pricing of the services they receive. Patients visit doctors who receive payment from third parties. As health insurance plans shift more payment responsibility to policyholders, individual consumers confront ever-higher healthcare bills.
Half of all Americans have annual out-of-pocket costs exceeding $1,000 (1), while two thirds of all American don’t have that much in cash savings.(2) It should be no surprise, then, that some forgo treatment when they fear they cannot afford it.
Consumers have no idea how much healthcare services cost, and there are no pricing benchmarks to make meaningful comparisons across competing providers. Indeed, it isn’t until they receive a bill that most patients learn their portion of the cost.
Patients struggle to make sense of bills from multiple providers for a single treatment, sometimes different bills for different amounts for the same service from the same providers. Bills may arrive months afterward. Providers may send bills to collections before patients have the whole picture. Collection timing does not change for explanations or appeals.
The current payment system is dysfunctional. Payment rates for copays and deductibles are dismal. Unexpected healthcare costs and lost income during treatment are the leading contributors to personal bankruptcy in America.(3) Costs, payments, and billing do not center on the people receiving the care. Americans want more transparency and accountability for healthcare purchases.
Healthcare consumers feel the current payment and billing system treats them like patsies rather than patients. Fear of costs, not just fear of outcomes, stresses patients considering treatment options. Four in ten people are concerned about their ability to pay for care if they get seriously ill; one in three are very afraid about the economic effects of getting seriously ill.(4)
The current system feeds these fears. Payers, especially commercial insurers, can’t or won’t say how much they will pay for a procedure before it has been completed and billed; many won’t even give the average cost in a patient’s area.
Nobody likes surprises. Patients want to pay their fair share, but they want to know upfront what their payment obligations costs will be, not after the fact.(5) Healthcare payment mechanics generate financial uncertainty and stress. Absent information, patients worry about their ability to afford treatments and may forgo them for this reason. Providing services at a price that patients cannot understand or afford is no way to run a successful business. Write-offs can be significant. Shifting just 1% of receivables from insurers to patients lowers operation margins by 14%. (6)
Frustration often turns to anger. A bad payment experience negates the positive customer experience generated by successful treatment. Making payment more patient-centric is an essential component of generating brand strength for health systems.
MARKET SIGNALS
Throughout healthcare, consumers are demanding better care, better outcomes, better convenience and a better experience. Consumers expect healthcare to match the service, ease and value they experience in other areas of their economic life. They want better care access and clearer measures of quality. They want flexible payment terms and methods, including phone, online, in person, cash, check, credit, and HSA/FSA.
Most of all, patients want transparency. Patients want to know costs before treatment. They want the ability to talk to people who understand and can explain billing. They want the same respect and the same deference they get from other social and technological systems.
Despite a clarion call for change from patients, the healthcare system still resists change. Why? The reality is that the healthcare system we have is built on systems and practices for patients of 50+ years ago. Providers accustomed to Fee-For-Service are not prepared to tell patients what services they will order or what those services cost. As a result, there can be no transparency on actual costs. Provider organizations remain focused on their relationships with payers, offering different pricing models to different insurers. They wait for third-party reimbursements before telling patients what their share will be.
But the weaknesses of the current system are impossible to ignore. Many providers now collect a lower percentage of billing. Revenue is unpredictable. Costs of collection, whether with inhouse staff or outside vendors, subtract from provider revenue. Patient satisfaction and loyalty drop, and with it the strength of the patient/provider relationship.
Infuriating and scaring customers are not required steps in the delivery of healthcare services. Farsighted providers see an opportunity to gain market share by getting customer payment right – by making it easy for customers to understand and pay healthcare bills.
THE PRICE IS RIGHT
 Consumers reward quality and service by choosing plans and providers that appeal to them. Smart providers know that increasing patient satisfaction increases patient loyalty. Exemplary billing and payment dramatically increase the numbers of patients who will recommend a hospital to a friend or relative.
Consumers reward quality and service by choosing plans and providers that appeal to them. Smart providers know that increasing patient satisfaction increases patient loyalty. Exemplary billing and payment dramatically increase the numbers of patients who will recommend a hospital to a friend or relative.
Patients are twice as likely to pay in full if they are satisfied with the billing process, and five times more likely to recommend the hospital if they are “very satisfied” with their financial care.(7) Successful healthcare payment programs incorporate the following 5 elements:
- Clear communications
- Flexible payment scheduling
- Convenient payment methods
- Cost transparency
- Easy to navigate payment mechanics (enabled by technology)
 AdventHealth (AH) chose to invest in its patients’ financial care, changing that dynamic for the 5 million+ patients served annually. With nearly 50 hospital campuses spread across nine states, complemented by almost 20 skilled nursing facilities and over 20 home health and hospice agencies, AH serves patients with complicated care and the related financial situation. Since “Affordable” is one of the five components of the system’s vision, and “Make It Easy” is one of the core service standards, the focus on financial care is critical to AdventHealth’s purpose.
AdventHealth (AH) chose to invest in its patients’ financial care, changing that dynamic for the 5 million+ patients served annually. With nearly 50 hospital campuses spread across nine states, complemented by almost 20 skilled nursing facilities and over 20 home health and hospice agencies, AH serves patients with complicated care and the related financial situation. Since “Affordable” is one of the five components of the system’s vision, and “Make It Easy” is one of the core service standards, the focus on financial care is critical to AdventHealth’s purpose.
Many systems want their revenue cycle management to be customer-centric, and many identify different aspects required. AdventHealth decided to achieve that customer focus, they must offer:
- Self Scheduling
- Single, Enterprise-wide Bill
- Mobile Scheduling
- Self-service Pre-registration
- Mobile Pre-service Payments
AdventHealth turned to Simplee, a company that works with providers to develop more patient-focused billing and registration systems. A Simplee-designed system now provides AH customers with a single bill for all services – one that clearly identifies patient payment obligations – and the unified billing experience provides multiple payment options.
The Simplee system, white-labeled for AdventHealth, gives customers the information they need to pay their bills and the flexibility to make those payments in the most convenient way. Patients comment on both the integrated bill itself, as well as the ease of use of the website and mobile application. In fact 78% of payments are now self service, with 29% of the online payments coming through mobile.
 “I have a passion around making the consumer experience in revenue cycle much more delightful for our patients. Patients really do seek the self-service experience and that’s what we’re offering.”
“I have a passion around making the consumer experience in revenue cycle much more delightful for our patients. Patients really do seek the self-service experience and that’s what we’re offering.”
Timothy Reiner, SVP Revenue Management, AdventHealth
Another key component of the AdventHealth payment system is the flexibility offered in payment plans. Short-term payment plans don’t work for the 50% of bills with high balances, since 9 of 10 patients say a healthcare expense requires financing for more than 12 months. Using predictive patient data and a financial scoring algorithm tuned for healthcare, the AH billing system presents a path to payment that matches patient needs. AH sees twice as many patients creating their own plan, and many customers expressing appreciation for the flexibility.
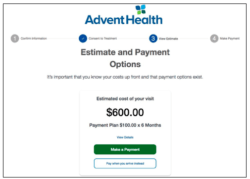 While these payment system advancements have made great strides after patients receive care, AdventHealth understood the importance of registration in a patient’s overall experience, as well as its tie to financial care. AH is partnering with Simplee to rethink healthcare visit registration, taking a page from the airline industry where customer check in now happens almost entirely via mobile devices. AH’s new patient registration experience allows a patient to complete check-in tasks like confirming data and reviewing consent forms from their phone, rather than while sitting in a hospital waiting room. The experience also allows a patient to see an estimate of their out-of-pocket costs and payment options – all without having to call an AH staff member.
While these payment system advancements have made great strides after patients receive care, AdventHealth understood the importance of registration in a patient’s overall experience, as well as its tie to financial care. AH is partnering with Simplee to rethink healthcare visit registration, taking a page from the airline industry where customer check in now happens almost entirely via mobile devices. AH’s new patient registration experience allows a patient to complete check-in tasks like confirming data and reviewing consent forms from their phone, rather than while sitting in a hospital waiting room. The experience also allows a patient to see an estimate of their out-of-pocket costs and payment options – all without having to call an AH staff member.
By investing in patient financial care, AdventHealth has improved its own success metrics. Self-service payment and payment plan originations are growing, with an 85% repayment rate. The AH revenue cycle experience has a net promoter score of 40, compared to the average healthcare billing office score of 18.(8) AH has also reduced staff time needed for registration and payment issues, and seen a meaningful decrease in collection costs. Win for the patients, win for AdventHealth.
A CROWNING ACHIEVEMENT
Queen Elizabeth heeded the “market signals” and placed the British people at the center of her programs for the monarchy. She made this transformation with grace and humor.
The Beatles performed a high-profile royal concert in 1963 with the Queen and the Court in attendance. Before playing their final song (“Twist and Shout”), John Lennon asked those in the cheaper seats to clap with the music and the rest to “rattle their jewelry.” (9) No talk of drudgery this time. The Queen smiled and went along with the gag.
 Queen Elizabeth II is the longest-reigning monarch in British history. At 92 years of age, she is in the 66th year of her reign and shows no signs of slowing down. Without her adaptability, it could have turned out differently for the British monarchy.
Queen Elizabeth II is the longest-reigning monarch in British history. At 92 years of age, she is in the 66th year of her reign and shows no signs of slowing down. Without her adaptability, it could have turned out differently for the British monarchy.
Happy customers are paying customers. Enlightened health systems are heeding current market signals from American healthcare consumers. They’re transforming their operations to provide higher-value services and better customer experiences. Those that pivot successfully will gain market share, mindshare and longevity. Long live high-value healthcare.
SOURCES
- Kaiser Family Foundation: 2016 Employer Health Benefits Survey (14 Sep 2016) and US Dept H&HS (2016 survey)]
- USA Today “Nearly 7 in 10 Americans have less than $1,000 in savings” (9 Oct 2016)]
- https://www.washingtonpost.com/blogs/post-partisan/wp/2018/03/26/the-truth-about-medical-bankruptcies/
- webinar min: 4:55 West Health Institutes / NORC poll of 1302 adults Feb 2018
- InstaMed 2016 Trends in HealthCare Payments, May 2017]
- Analysis of average $1NPR US Hospital system facing shift of revenues billed from insurance payers to patients and corresponding impact on op mar gin holding other factors constant
- Longitudinal study of patient satisfaction with billing and payment experience by Connance (Consumer Impact Study, 5th annual, results published Aug 2014, sample size n=500)]
- AdventHealth NPS based on 42,494 patient responses. Healthcare average from Longitudinal study of patient satisfaction
with billing and payment experience by Connance (Consumer Impact Study, 5th annual, results published Aug 2014). - https://www.youtube.com/watch?v=rvBCmY7wAAU
CO-AUTHOR
 Tomer Shoval is the CEO and Co-founder of Simplee. Tomer was inspired to start Simplee after experiencing his own struggle trying to decipher family medical bills. Coming from a background in digital experience from his years at Shopping.com, the first internet shopping comparison site, Tomer saw an opportunity to bring a similar consumer-centric mindset to the patient financial experience. He founded Simplee in 2010 to pursue the mission of eliminating the stress of financial care so that patients can focus on their well-being.
Tomer Shoval is the CEO and Co-founder of Simplee. Tomer was inspired to start Simplee after experiencing his own struggle trying to decipher family medical bills. Coming from a background in digital experience from his years at Shopping.com, the first internet shopping comparison site, Tomer saw an opportunity to bring a similar consumer-centric mindset to the patient financial experience. He founded Simplee in 2010 to pursue the mission of eliminating the stress of financial care so that patients can focus on their well-being.